Period Pain: Could It Be Endometriosis?
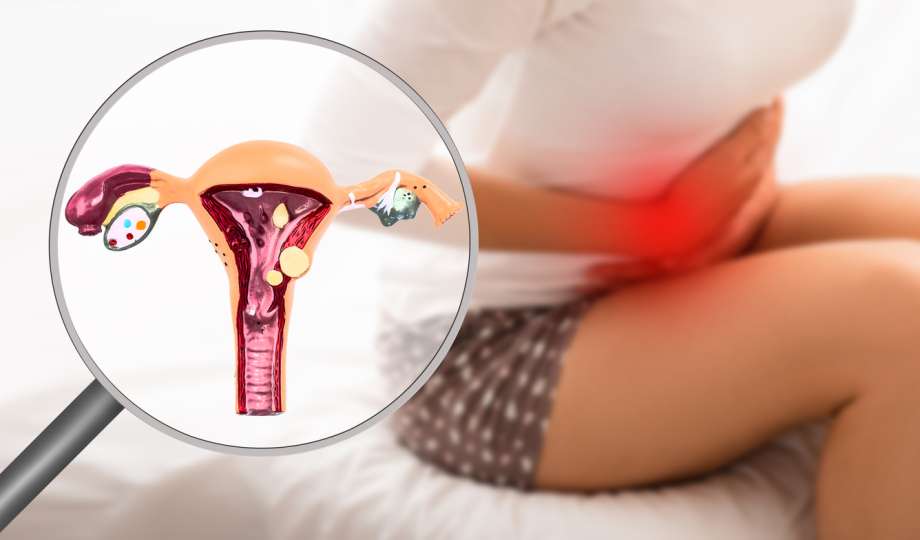
“It’s normal.” That intense, pulsing pain that radiates throughout your abdomen every single month has been deemed as a regular part of womanhood. Most of the time girls are told to buck up, take some ibuprofen, and go about their day. However, this extreme discomfort could be an indicator of a more serious issue. We take a look at the differences between period pain and endometriosis and what to do if it is the latter.
What is Dysmenorrhea?
Dysmenorrhea is the fancy word for menstrual pain. This can range from mild to extreme discomfort. Unfortunately, painful periods are a stereotypical part of a woman’s monthly cycle. Nonetheless, it is important to note that there are two categories of this condition.
Primary dysmenorrhea begins when an adolescent female starts menstruating. This level of pain continues throughout her reproductive years with no drastic changes over time. These cramps can be intense, but usually only occur right before and during her period.
Conversely, secondary dysmenorrhea refers to when a woman’s menstrual cramps worsen later in life. This is likely due to an underlying condition. These can include ovarian cysts, uterine fibroids, pelvic inflammatory disease, the use of an IUD, or endometriosis.
What is Endometriosis?
Every month, a woman’s body produces a mucous membrane called endometrium that lines the inside of the uterus. This uterine lining is where the embryo will attach itself to if you become pregnant. However, if implantation does not occur, the lining will shed during your monthly menstrual cycle. Unfortunately, for some women, this lining forms in the wrong place — often over the reproductive organs (more specifically, the fallopian tubes and the ovaries). Although it can grow anywhere in the body.
According to the Mayo Clinic, “with endometriosis, the endometrial-like tissue acts as endometrial tissue would — it thickens, breaks down and bleeds with each menstrual cycle. But because this tissue has no way to exit your body, it becomes trapped.” This can cause intense pain, excessive bleeding, and even infertility. Moreover, since these symptoms usually occur at the time of menstruation, it is normally misdiagnosed as period pain.
A Misdiagnosis is Much More Common Than You Think
Research shows that an astounding “75.2% of patients reported being misdiagnosed with another physical health and/or mental health problem.” Furthermore, as of 2020, the average time it took to acquire the correct diagnosis of endometriosis was 8.6 years. This means that millions of women in the United States are not being properly treated for a chronic condition that occurs every single month of their reproductive years.
This leads many to question if their intense pelvic pain is related to their period or if they have a more serious condition. Let’s break down those differences and provide you with information on how you can proceed if you think that you may have endometriosis.
Causes of Endometriosis
The exact cause of endometriosis is unknown, but it is theorized that retrograde menstrual flow is the main trigger. This is where some of the endometrium moves in the wrong direction and is transported back into the abdominal cavity. This allows these cells to stick onto areas where they don’t belong. The cause of this condition is also unclear, but anatomical anomalies could be the reason that some women are more prone to this issue.
Additionally, while there is still a lot more research that needs to be done, studies show that this condition does run in families. This may not seem like a relief, but it does allow those with a proper diagnosis to warn other family members that they could be at risk. This, in turn, allows for earlier interventions, and therefore, an overall better quality of life for those individuals.
Common Symptoms of Endometriosis

As mentioned, severe pain before and during menstrual periods is the first sign of this condition. This cramping will occur throughout the abdominal cavity with many women noting lower back pain as well. However, some women do not report endometriosis pain, so it is imperative that you look for less obvious symptoms as well.
These can include heavy menstrual bleeding, and many times, bleeding that occurs in between menstrual cycles. Clots may also be expelled during these bleeding events. Furthermore, other signs of endometriosis include pain during urination, bowel movements, sexual intercourse (otherwise known as dyspareunia), and even tampon use. Women also note that this condition impacts their gastrointestinal health, causing constipation, diarrhea, nausea, and bloating. The term ‘endo belly’ is used all over the internet, with many women posting pictures of their swollen abdomen in support of one another with the condition.
Diagnosis of the Condition
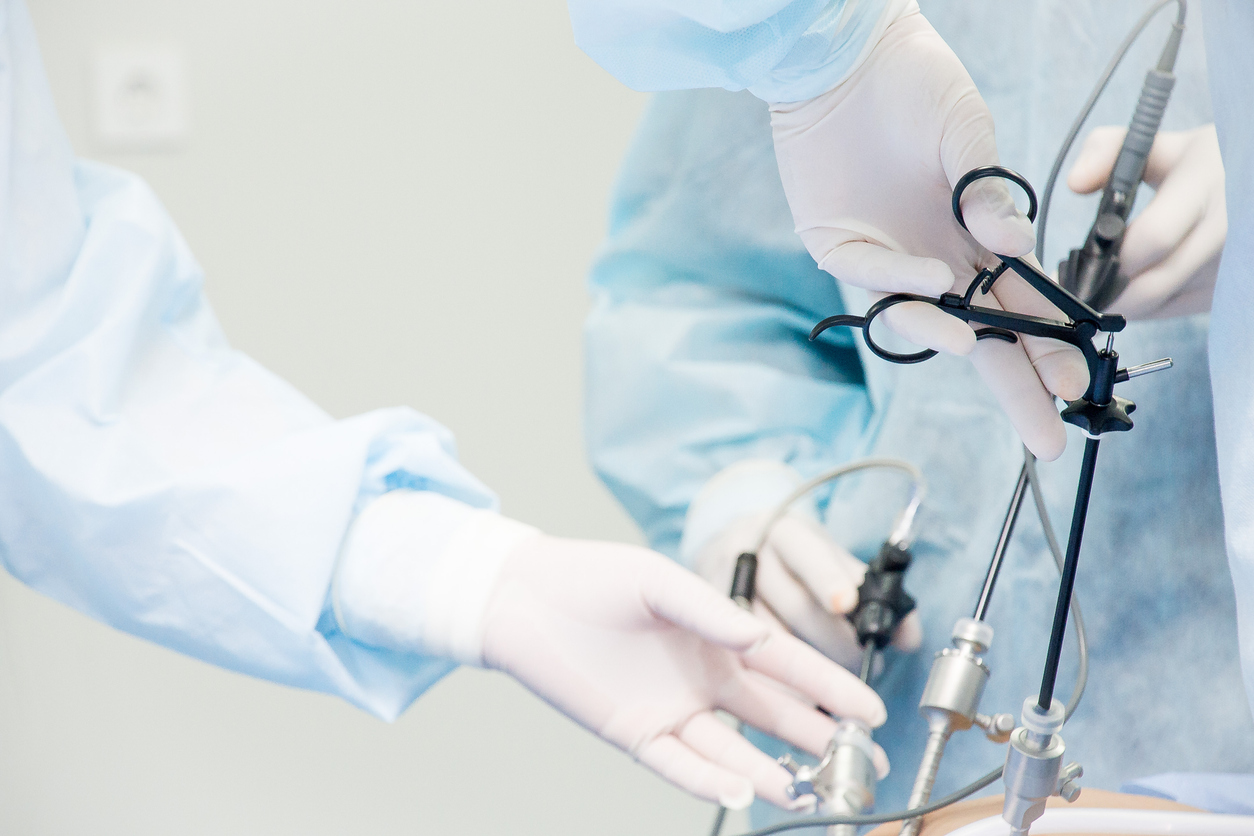
The diagnosis of endometriosis can be very difficult. While a pelvic exam may indicate to a gynecologist that you could have this condition, the only way to definitively confirm this hypothesis is to conduct a laparoscopic procedure. This is performed through one to a few small, key-hole incisions into the abdomen.
Sadly, many women receive an endometriosis diagnosis when struggling to conceive. One of the complications of this condition is infertility. Theories suggest that this occurs because the endometrial tissue that has formed in the wrong area can prevent the egg from meeting with the sperm, but far more research is needed.
The chances of endometriosis worsening increases with each cycle as more tissue forms within the pelvis. This is why paying attention to symptoms and advocating for yourself are the two most important steps in receiving an accurate and early diagnosis. Therefore, if you suspect that you may have endometriosis, contact your OBGYN and set up an appointment to discuss your concerns. There are OBGYN’s who specialize in infertility and endometriosis. Talk to your healthcare provider about your options - it’s important to find someone you trust and feel comfortable talking to.
Treatment Options Depend on Severity
The course of treatment for this condition is dependent on the severity of your endometriosis. For mild cases, treatment options include over the counter pain relievers and hormonal contraceptives (like birth control pills) to help control your hormone levels. However, if you have a more severe case, surgery may be required to remove growths, cysts, and scar tissue.
Unfortunately, if symptoms are extremely severe and the condition is left untreated for too long, a hysterectomy may be recommended. This is an extreme treatment plan that will remedy all of your symptoms, but it will also bring on early menopause, which can be a big adjustment.
Again, a timely diagnosis is key, so listen to your body and speak up when you have concerns! Period pain is normal, but it should never impede your ability to function on a day to day basis.
Where to Find Support

Finding out that you have endometriosis can be overwhelming, especially since there is no cure. However, there are organizations like the Endometriosis Foundation of America and SpeakENDO.com that rally to encourage more medical research, and provide emotional support for those who suffer with this debilitating condition.
You can also talk to your doctor about support groups and local resources to help you cope with endometriosis. Finally, it is important to remember that you are not alone. 10% of women have endometriosis, making this a major women’s health issue. Celebrities such as Halsey, Chrissy Teigen and Emma Roberts have all been vocal about their experience with endometriosis and have inspired many more women to come forward and spread awareness.
Staying quiet only silences the problem and furthers the stereotype that the term ‘endometriosis’ simply means ‘bad period pain.’ For every woman that comes forward and shares their story, another step is taken in re-educating the world regarding what is normal and what is not when it comes to period pain.

