I'm Having a "Geriatric Pregnancy." Am I Really At Risk?

There are many things that could use a facelift within the birth world, but one of the most disturbing things to me is the language that is used to speak to and of pregnant people. It’s absolutely incredible the level of disrespect and twisted thinking passed down in the mere way we talk about pregnancy and the entire reproductive journey. Our medical system has diagnostic words like "failure to progress," "failure to thrive," and "incompetent cervix." These terms are not reserved for the worst of the worst either. No, these words that sting like acid in a wound are thrown around labor rooms as easy as casual greetings. It's no wonder why women have such a hard time mentally with transitioning to motherhood once they've been told their body is essentially broken, in not so many words of course.
More: TTC? 5 Things to Consider First
What is a "geriatric pregnancy"?

One of the terms that irks me the most is geriatric pregnancy. This less than endearing term insinuates that a woman is old at the age of 35 years old. The word geriatric, by definition, means relating to old people, especially in regard to healthcare; a branch of medicine that specializes in the care of problems and disease of old age.When I think of the word geriatric, I think of an elderly folks home with truly geriatric people, not a flourishing and healthy 35-year-old woman healthy enough to sustain life for two humans (hers and the baby in her belly). The term "advanced maternal age" is slowly becoming the new PC way of saying "older pregnancy," but honestly you don't have business commenting on someone's age and pregnancy if you aren't their doctor.
*Trigger Warning: this article talks about risks to AMA (Advanced Maternal Age) pregnancies including infant loss.
Can I get pregnant after 35?

Other than the actual words "geriatric pregnancy," this label is a blanket label that can drastically impact someone's birth experience based on the single factor of age. If you are required to have unnecessary monitoring or testing based on your age alone, this may disrupt your birth in more than one way which has the potential to drastically change the outcome. This is where finding a provider who supports your plan and desired birth story is really, really important.
A geriatric pregnancy is classified as a pregnancy that occurs in a woman over the age of 35. It does not, however, take into account the woman's current health, previous health, exercise, diet, family history, or access to resources. ACOG, or The American College of Obstetrics & Gynecology, states that a woman's chance of getting pregnant in her 20's is one in four, but declines to one in ten by the time she is 40 years old. They explicitly state that fertility is "unlikely" after the age of 45. But, don't let this be discouragement! There are millions of women walking around everyday that have successfully carried a healthy pregnancy to term and given birth safely and gently to a healthy baby.
Professor and Author of Expecting Better, Dr. Emily Oster explains that her findings revealed women who got married between 35-39 years old have a 90% chance of having a child. Women who get married between 40-44 years old have a 62% chance. However, women who got married after 45 years old only have a 14% chance of having a baby.
Is it really that scary to be pregnant and 35+?
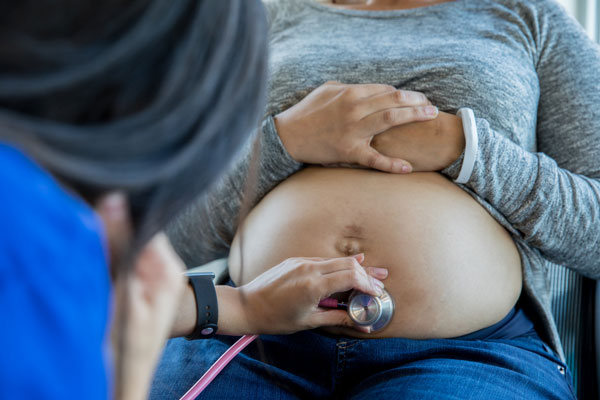
I chatted with Jocelyn Brown, a Licensed Homebirth Midwife in Los Angeles, California, on the truth about older pregnancies. She shared, "Having a geriatric pregnancy is nowhere near as scary as it sounds. While statistics indicate that certain complications may be more likely for women over 35, most of the risks can be reduced by starting your pregnancy in good health, getting excellent care, getting good nutrition and exercise, and following your care provider's recommendations for testing. About half of my clients are 35 or older, and there's research that indicates that women over 35 and their babies have excellent outcomes in out-of-hospital midwifery care."
Are there risks? Of course! There are very little things in life that have zero risk. But, honestly, there's not much risk based on your age alone. Unless you have another condition that would be a cause for concern, you shouldn't have anything to worry about based solely on the number of years you've been alive.
However, women over the age of 45 do face a few more challenges, but none are guaranteed just because your are 35+. The common thought is that the older you are, the less efficient your downstair machinery works. While this may be true, there's also a lot of hype out there that you might be surprised to find isn't all that true!
No matter what, every pregnancy will carry a certain level of risk. The key is evaluating those risks and understanding what's a relative risk and what's a fear-based risk. Here are a few complications that commonly arise for women over 35 years old and pregnant.
More: The Benefits of Delayed Cord Clamping After Birth
What exactly are the risks of advanced maternal age pregnancies?

Down Syndrome
This is, by far, the most common "complication" that people associate with older pregnancies. At the age of 35, you have a 1 in 353 chance of giving birth* to a child with Trisomy 21. By the time a woman is 40 years old, the odds of having a child with Down Syndrome has increased to 1 in 85.
*Due to high rate of miscarriage, the rates of conceiving a child with Down Syndrome is slightly higher than the number of babies born with Down Syndrome
Miscarriage
By now, you must know that the statistics for miscarriage are astonishing. Research findings show 25% of women will experience a miscarriage at some point in their life. And, there is no doubt that as women age, their risk of miscarriage increases as well. At the age of 22, a person's risk of miscarrying is only 9%. However, at the age of 30, the risk has doubled to 18% and by the time your 40th birthday comes around, your chances of miscarriage has skyrocketed to 40% and increases to nearly 50% by your 50th birthday!
Gestational Diabetes
A "typical pregnancy" of someone 35 years old or younger has a 1% risk of developing gestational diabetes. For someone who is between the ages of 35-40 years old, the risk rises to 2.9%. After the age of 40, it increases to just over 4.5% of pregnancies. This diagnosis has the potential to increase your chance of induction according to ACOG.
Preeclampsia
This is a condition, often after the 20th week of pregnancy, where pregnant people experience high blood pressure, a presence of protein in their urine, and sometimes swollen hands and feet. The risk of women over the age of 40 is almost twice that of women 35 years old. In general, preeclampsia only impacts 5-8% of pregnancies. There are a few factors that may increase your risk of developing GD and those are age, first pregnancies, having a family history of GD, pregnancies carrying multiples, having a BMI of 30 or higher and among a few more things.
Challenges with your Placenta
According to Evidence Based Births, the general population of pregnancies carry a risk of 0.26% chance of experiencing placenta previa, a condition in which the placenta attaches in a position that is too close to, even covering, the cervical opening for a safe vaginal delivery. For women between the ages of 35 and 39 years old, the rate increases to 0.56% and is nearly one whole percent (0.97%) for women 40 years and older.
Stillbirth
The risk of stillbirth increases with the age of the gestational parent. However, it's quite small and ranks just above the general risk. Evidence Based Births shares research in the UK that studied over 350,000 women and found 6.1 out of every 1,000 people (equalling 0.61%) over the age of 35 will experience a stillbirth. The study also found that women over 40 years old had a 0.81% of experiencing stillbirth.
Cesarean Birth
The C-section rate in America is between 32 and 33% and for women over 35 years old, they face an astounding rate of up to 39%. For women 40+ years old, the rate climbs. However, when we look at other countries, we do not see this trend. This study in Australia shows that women who are pregnant at 38 years old have no different cesarean rates than women pregnant younger than 38 years old.
The Bottom Line?

If you are over 35 years old, you may experience a more difficult, but not impossible, time trying to conceive. If you are older than 45, your chances are slimmer, but still not impossible. You can receive care from an Advanced Maternal Age Specialist who knows how to properly support you. You can have a very normal and gentle pregnancy and birth experience while still being over the age of 35. Advanced Maternal Age pregnancies can be managed with a supportive and hands off approach if you eat well, exercise regularly, do not smoke, and receive routine prenatal care by a qualified professional.
To include every single woman 35 years old and older in one category and require them all to have specialized maternity care certainly seems like an unnecessary step, but so often one that healthcare providers are not willing to budge on. If you are confident in your own health, your family history, and your ability to navigate your options, then it's worth searching (and possibly traveling for) a provider that aligns with your birth expectations.
Rebecca Dekker, PhD, RN, APRN, and founder of Evidence Based Births shares, "There is no consensus among researchers and obstetrical/midwifery organizations on the best way to care for a person at the end of pregnancy when they are 35 or older. As we gain more research on this topic, perhaps we will have better guidance. However, the good news is that the vast majority of people 35 and older who make it to term will have a healthy baby. Intervention rates for this group may be further lowered by using a midwifery-led model of care."
I'll leave you with this: Age is just a number and you know your body best. Maintain a healthy recognition and respect for your providers knowledge and balance that with knowing your rights as a patient and your goals for your ideal birth.

