The Covid Booster Pregnancy Guide for Winter

The gestation period is a fragile time for both a mother and her developing baby. It is a period of reduced immunity and overall body defense for the mother, and the immunity of the baby is not yet developed. It is made even more fragile by the fact that over the last couple of years, the world has had to battle a deadly pandemic that majorly affects those with reduced immunity against infections and diseases.
The winter period also contributes to this low immunity, especially for pregnant mothers. Therefore, many would need to shore up their immunity by getting vaccine boosters to help them and their baby stay healthy through the cold season.
COVID-19 Risks for You and Your Baby

It has become increasingly clear that COVID-19 is not a once-in-a-lifetime disease; it has become an endemic disease with different variants that become more resistant as they progress. It is, therefore, important to be wary of getting infected by any of these resistant variants as a pregnant woman.
According to the Journal of Infectious disease, COVID-19 predisposes a pregnant woman to a range of severe complications, ranging from invasive ventilation to death. While for the baby, there is an overall very low risk of mother-to-child transmission of the virus, this risk has, however, increased with each successive variant, alongside other pregnancy complications such as preterm birth or stillbirth.
Unvaccinated and partially vaccinated mothers also have a high risk of hospitalization when infected with the virus. This risk increases considerably during winter, especially if there is the superimposition of other viruses, such as influenza, that are able to take advantage of the immunocompromised state of the mother.
Other health conditions that risk the health of pregnant women and predispose them to infection and complications from COVID-19 include comorbidities such as diabetes, heart disease, and asthma. Women over 35, overweight women, and women in certain minority groups also have a higher risk of infections and complications.
Currently, several FDA-approved clinical trials are going on to create a cure for the coronavirus infection, especially for people with severe illnesses or under intensive care; however, the best course of action is to boost immunity to prevent infection or possible hospitalization.
While these facts may be frightening, there are steps you can take to boost your immunity and ensure your and your baby’s safety.
What Should Pregnant People and Breastfeeding Mothers Do?
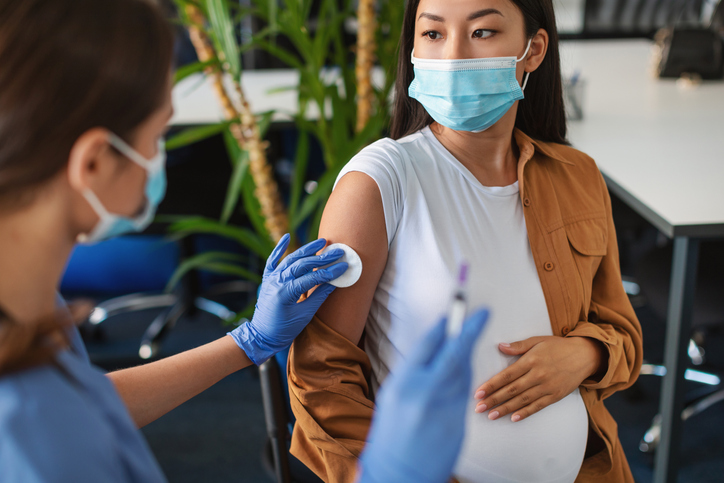
At FamilyEducation, we know that women across the board are on a vaccination spectrum for various reasons, from no vaccination to three doses. However, following what we have mentioned above, it is okay to get the vaccination in your own time, whether you’re planning to get pregnant or are in any of the three trimesters. If you have been vaccinated, it is okay to get boosted.
According to the Royal College of Obstetricians and Gynaecologists, anyone trying to get pregnant does not need to avoid the vaccine or a booster, as the vaccine does not affect fertility.
Pregnant people are considered immunocompromised and therefore have an increased risk of severe COVID-19 infection. Although the CDC advises that everyone from 5 years old, regardless of whether they are immunocompromised, should receive one updated booster dose, it is especially important for pregnant people to receive an updated COVID-19 booster to help restore protection that has waned since their last vaccination.
When receiving the Moderna or Pfizer-BioNTech series, the CDC recommends that most moderately or severely immunocompromised persons receive an additional primary series dosage.
Pregnant women are also advised to get vaccinated or get boosted regardless of their trimester; this will improve their immunity and protect their baby through the coming winter. A study that was reported by U.S.News showed that 78% of babies born to vaccinated mothers have antibodies to SARS-CoV-2, the COVID-19 virus. This amount is expected to reduce by 6 months of age due to the weaning of maternal immunity from the children in this age group over time.

The Journal of Infectious disease published a report where the researchers noted that complete vaccination during pregnancy could help prevent COVID-19-related diseases amongst infants that are less than 6 months of age.
COVID-19 vaccinations provide excellent disease protection; however, the level of protection diminishes over time. Even if you have already received COVID-19 vaccines or are infected with the disease, the autumn booster is necessary to keep you and your baby safe throughout the upcoming winter months, when disease levels are predicted to rise. Currently, the American Academy of Pediatrics reports show that 18.3% of all COVID-19 are children and infants. Hence, getting vaccinated is best to give your baby a head start in immunity.
You can also read through our guide to navigating the winter as a pregnant person for steps to take and precautions to follow.
Speak With Your Healthcare Provider
The importance of speaking with your physician throughout pregnancy cannot be over-emphasized. It has become even more essential with the current COVID-19 infections; therefore, you need to get in touch with your health provider on major issues such as vaccine safety to keep you and your baby healthy during pregnancy.
Whether you’re taking it for the first time or you’re having a booster shot, your doctor will have details of your previous history vaccination records.
What COVID-10 Vaccine Can You Get?
As winter approaches, there is a possibility of increased demand for the COVID-19 vaccine. This, along with other factors, would determine the availability of the vaccine for those seeking their first-time vaccination and those who have received two doses seeking a booster dose.
Other things that may affect what vaccine you receive include the vaccine available at your location, your previous vaccinations, possible side effects, and the current variant that you’re being vaccinated against. In some cases, combination doses are made available due to their effectiveness against a circulating variant.
In the United States, the CDC has approved four types of vaccines for use. They are; Pfizer-BioNTech and Moderna mRNA COVID-19 vaccines, Novavax COVID-19 vaccine, and Johnson & Johnson’s (Janssen (J&J/Janssen) COVID-19 vaccine. The Process of vaccination is being monitored by the vaccine adverse event reporting system.
Each Vaccine Explained
Pfizer Vaccines are mRNA vaccines. This means that unlike other vaccines, which contain live viruses or weakened and inactivated viruses, mRNA vaccines use mRNA that is generated in a lab to train our cells how to make a protein or a part of the protein that prompts an immune response within our bodies. This immune reaction, which creates antibodies, is what protects a person against future infection. This also applies to Moderna Vaccines.
The Novavax vaccine is a protein subunit vaccine that contains fragments (proteins) of the virus responsible for COVID-19. The vaccination also contains an adjuvant, which improves the immune system's response to the spike protein in the future. Once your immune system has learned how to respond to the spike protein, it will be able to respond swiftly to the genuine virus spike protein and protect you from COVID-19.
The Johnson Vaccine is a viral vector COVID-19 vaccine. It uses a modified version of another virus to deliver important instructions to our cells and confer immunity.
All these vaccines have undergone clinical trials and are authorized for use by the U.S. Food and Drug Administration, and they are also being continually monitored for safety concerns.
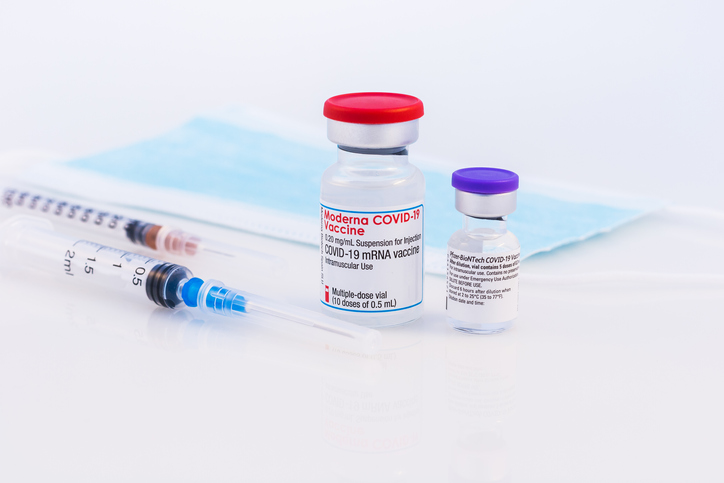
The vaccine series that allows you to complete your vaccination differs for each of these vaccines. This implies that some of these vaccines require two doses while some require a third dose. Some do not require an additional dose after the first dose, like the Johnson vaccine, for people who are 18 years old and above.
You may be offered an enhanced bivalent version of these booster vaccinations, which include a component of the original virus strain to provide wide protection against COVID-19 and a component of the omicron variant to provide improved protection against COVID-19 induced by the omicron version. Because they contain these two components, these vaccines are known as bivalent COVID-19 vaccines. Both the prior and combo vaccines provide excellent protection, with the combination vaccine producing somewhat higher levels of antibodies against particular strains of Omicron.
A doctor may recommend another vaccine product for a very small number of people; for example, if the first dose was AstraZeneca, pregnant women are usually advised to take the same vaccine for their second dose.
The most important thing is to speak with your physician to help you decide on which vaccine is best for you. Women are encouraged to take the booster doses that they are offered.
In addition to COVID-19 vaccines, several other vaccines are important for pregnant women and their babies during the winter months, including the flu and whooping cough. These vaccines may be given together; however, there may be practical reasons to keep intervals between them.
Possible Side Effects

Vaccines work; however, getting the vaccine is not the end of it. You should be equipped with the knowledge of potential risks that come along with vaccinations, such as how many doses of the vaccine required and the common side effects. This, most of all, will prevent any form of apprehension when you experience the effects, and means that you’ll know how to engage in self care as soon as you see these signs.
Immune responses to the vaccine are different for each individual. However, tenderness and pain at the vaccination site, headache, tiredness, and mild flu-like symptoms are the most commonly experienced side effects. These symptoms do not generally last more than a week. Therefore, if your symptoms are extended, make an emergency call and stay at home.
Severe allergic reactions or anaphylaxis are not expected but could occur. If you feel chest pain, palpitations, swollen tongue, or shortness of breath, please call your physician or healthcare provider for specific instructions on what to do and how to report it properly.
Other vaccines that you might take can also affect your pregnancy, such as the flu vaccine, which the CDC has explained duly. You can also read about getting the TDap vaccine from our website.
So, to answer the question, do you need the booster vaccine dose as we approach winter as a pregnant woman? Yes, you do. Research has shown that an mRNA booster increases the immune response, improving protection against serious COVID-19 infection.
You should speak to your healthcare provider as soon as possible to determine the best course of action. They will always keep you updated about the Centers for Disease Control and Prevention guidelines.
Ultimately the decision to take the vaccine is yours; however, it is important that we provide you with the necessary information and equip you with the resources that will help you stay in touch with available vaccine information and the current trends as we approach the winter season.
Please check our website for further reading and FAQs about giving birth in the current COVID-19 pandemic.

